Osteoarthritis vs Rheumatoid Arthritis Differences: What Every Achy Joint Deserves to Know
Six months ago, a reader named Margaret emailed me in all caps: "MY HANDS ARE KILLING ME. Everyone says it’s arthritis—but my neighbor says she has osteoarthritis, while my doctor's talking about rheumatoid. Am I supposed to know the difference?!"
If you’re nodding along, you’re definitely not alone. I’ve been an orthopedic nurse for over 20 years, and I still see folks tripped up by these two forms of arthritis. They may share the same last name, but trust me: they’re as different as apples and oranges—and that matters, especially when you’re picking treatments or planning your day around pain.

Living With Joint Pain: The Real-World Headache
Let’s get real for a second. It’s not just a little stiffness or an occasional twinge. It’s the coffee cup you can’t grip at sunrise, the stairs that might as well be Everest, or the late-night ache that keeps you up. I watched my own mother-in-law try to button her blouse with hands so swollen, she almost gave up. And knee pain? I’ve lost count of the folks I’ve met who actually dread getting out of bed.
It’s frustrating, overwhelming, and sometimes—yes—a little scary. The specifics matter. Because the path to relief (and control) depends on which kind of arthritis has you in its grip.
So, What’s the Actual Difference Between Osteoarthritis and Rheumatoid Arthritis?
Here’s the thing: both can leave you feeling like the Tin Man after a rainstorm, but they’re driven by totally different forces inside your body. Let’s pull back the curtain.
Osteoarthritis (OA): The Wear-and-Tear Culprit
- Cause: OA is, at its core, mechanical. Think: years (sometimes decades) of your joints “miles on the odometer.” Cartilage—the slick, cushioning stuff at the end of bones—gets worn down over time, so bones start rubbing together. Ouch.
- Age of Onset: Usually 50 and up, but younger folks with injuries aren’t immune.
- Symptoms: Achy, stiff joints—especially after activity. Swelling is possible, but not extreme. Most commonly hits knees, hips, hands, and spine.
- Pattern: Often stays on one side (say, your right knee) and hits weight-bearing joints hardest. Morning stiffness tends to improve after 30 minutes or so.
- Progression: Slow, steady, relentless (but not typically dramatic overnight changes).
Rheumatoid Arthritis (RA): The Immune System Wild Card
- Cause: This one’s an autoimmune disease. Your immune system gets confused, attacks the lining of your joints (synovium), and triggers chronic, damaging inflammation.
- Age of Onset: Can strike at any age—including in your 20s, 30s, or younger (though most common between 30-60).
- Symptoms: Red, swollen, warm joints—often with pronounced morning stiffness lasting more than an hour. Fatigue, fever, or weight loss can appear long before you notice your knuckles swelling up.
- Pattern: Usually symmetric—if your left hand hurts, the right will soon join the party. Small joints in fingers and toes are usually first.
- Progression: Can flare up suddenly and cause joint damage in months if not treated aggressively.
Table: Quick Comparison
| Osteoarthritis | Rheumatoid Arthritis | |
|---|---|---|
| Cause | Wear-and-tear, cartilage breakdown | Autoimmune, synovial inflammation |
| Onset Age | 50+ | 30-60 (but any age) |
| Morning Stiffness | <30 min | >1 hour |
| Joint Pattern | Asymmetric, weight-bearing | Symmetric, small joints |
| Swelling | Mild/moderate, hard bony | Significant, soft, warm |
| Other Symptoms | Usually none | Fatigue, fever, malaise |
If you’re rubbing your knuckles right now, wondering which bucket you fit in: don’t self-diagnose. Your doctor can run blood tests (for RA markers like anti-CCP and rheumatoid factor), imaging, and do a physical exam. I’ve seen plenty of folks with both types, or even forms that don’t fit the traditional molds. Medicine is messy like that!
Under the Microscope: What’s Really Happening Inside Your Joints?
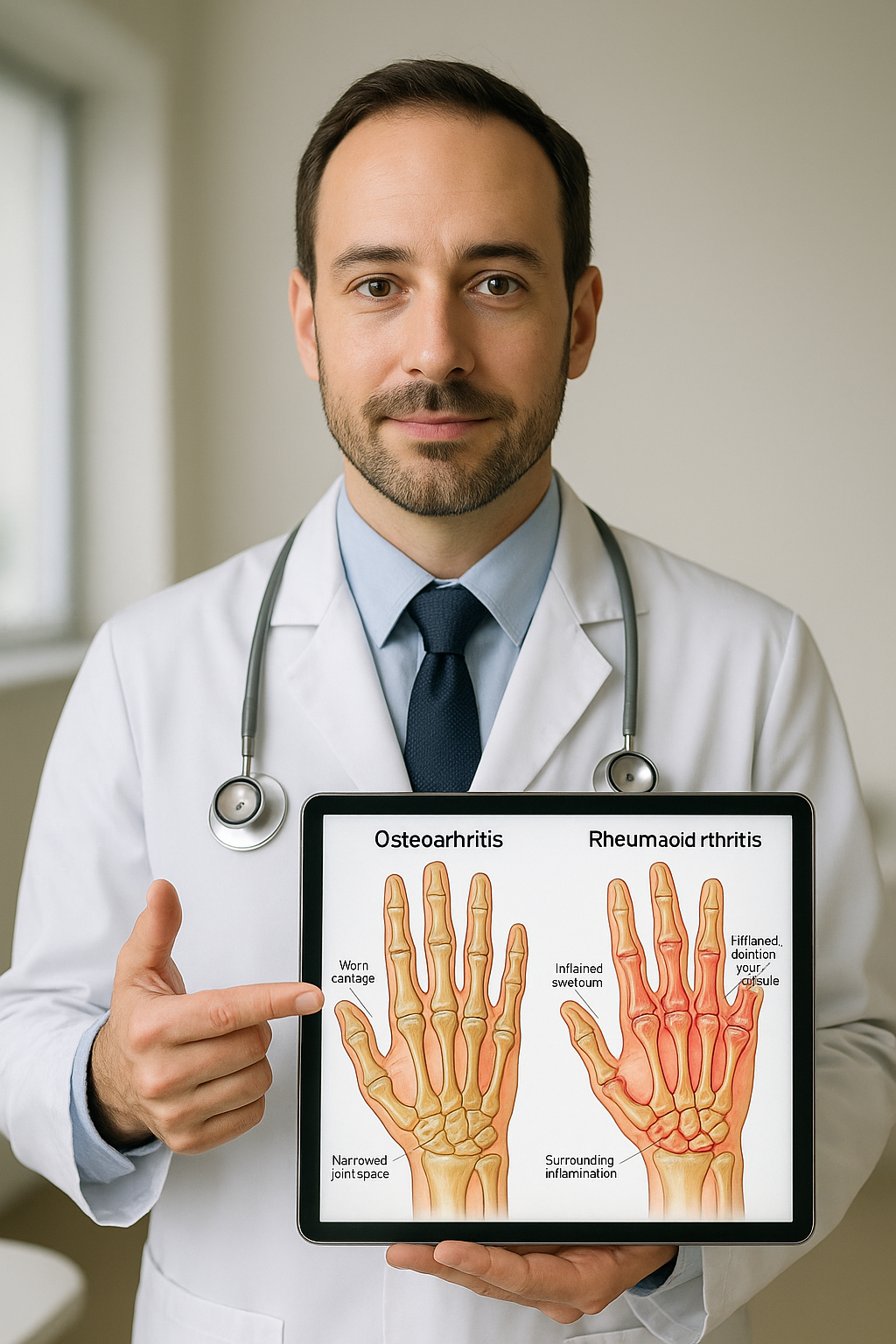
Here’s where it gets interesting—and honestly, a little humbling. Osteoarthritis is like the slow crumbling of a shock absorber in your car. Over time, the cartilage wears away, your bones start bumping into each other, and you might see bone spurs (osteophytes) on an X-ray. Pain comes from the loss of that protective padding.
Rheumatoid arthritis, on the other hand, is like your body’s security system going haywire, spraying fire extinguishers at perfectly innocent stuff. Your immune cells swarm into the joint lining, inflame it, thicken it, and can eventually erode cartilage and bone. That’s why RA tends to cause more dramatic swelling, and why untreated RA can destroy joints much faster.
There’s plenty of overlap, too. The Journal of Rheumatology (2021) notes up to 10% of older adults with RA also develop classic OA changes—so the plot thickens.
Treatment Paths: What Actually Works (and Why It Matters Which Type You Have)
This is the part that matters most for your everyday reality. Because the treatments for OA and RA are wildly different—and trying to “tough it out” with the wrong approach can mean years of unnecessary suffering.
Osteoarthritis: Strength, Motion, and Relief You Can Feel
I’ll be honest—when I first started out, I thought OA was a one-way street to joint misery. But the research says otherwise. The BMJ (2020) hammered home that targeted exercise and weight management can reduce OA knee pain by up to 40%. Not 5% or 10%. Forty.
Here’s what my patients (and my own knees) have found helpful:
- Consistent Movement: Gentle, regular activity—walking, cycling, swimming. Even 10-minute bursts matter. No marathons needed.
- Strengthening & Flexibility: I cannot overstate this. The right exercises stabilize the joint and reduce pain. My favorite? Treat Your Own Knees by Jim Johnson. It’s the only book I’ve seen that breaks down OA knee care into bite-sized, research-backed steps anyone can follow—no gym membership required. The diagrams are so clear even my Uncle Louie (who once called his hamstrings "the beef noodles") managed to follow them.
- Pain Relief: Topical NSAIDs like Voltaren Arthritis Pain Gel actually work, especially for knees and hands. The science isn’t wishy-washy; a 2016 Arthritis & Rheumatology review found topical diclofenac (the active ingredient) reduced pain better than placebo in OA, with very few side effects. I use it myself on marathon clinic days, and it’s saved me from reaching for oral painkillers. My tip: Apply it twice daily, give it a minute to dry, and don’t forget to wash your hands.
- Bracing: Soft, supportive braces can offload achy joints. I’ve seen good results with options like the NEENCA Professional Knee Brace for knees. The side stabilizers and gel pad really do make a difference for folks with instability or mild swelling. Just—please—don’t wear a brace 24/7; muscles need to work too.
And no, you don’t have to swear off stairs forever. Small, smart changes beat total inactivity every time.
Rheumatoid Arthritis: Calm the Fire, Save the Joints
Here’s where RA is a whole different beast. The main goal is putting out the immune system fire fast, before it scorches everything in sight. That means:
- Prescription Medications: Almost always required. This includes DMARDs (disease-modifying antirheumatic drugs) like methotrexate, hydroxychloroquine, or newer biologics. These target the cause, not just the symptoms. If your doctor suggests these, don’t panic—side effects are real, but so is the risk of untreated RA. I’ve seen lives transformed by the right cocktail.
- Physical Therapy: Range-of-motion and gentle strengthening help maintain function (and dignity). You may not love every stretch, but trust me: motion is lotion.
- Lifestyle Tweaks: Rest during flares, eat anti-inflammatory foods, and listen to your limits. It’s not about being lazy—it’s about protecting your joints while the meds take hold.
There’s one thing that frustrates me: I still see people with RA given only painkillers, and left to “see how it goes.” Unpopular opinion: That’s not good enough. Early, aggressive treatment changes the game.
What About Supplements, Injections, or “Natural” Cures?
I get asked about this at least four times a week. Glucosamine, turmeric, CBD—the list goes on. Here’s the honest scoop:
- Supplements: The evidence for glucosamine/chondroitin is mixed—2018 Cochrane review said “small to no benefit” for OA pain, but some patients do swear by 1500mg daily of glucosamine sulfate. For RA, there’s even less proof these work.
- Corticosteroid Injections: Can help with severe OA or RA flares, but effects are temporary and repeated shots can damage cartilage. Use with caution.
- Diet & Lifestyle: Losing 10 pounds can cut knee OA pain by 50% (per a memorable Arthritis Care & Research 2013 paper). And some folks with RA notice less pain when they cut processed foods or gluten, but there’s no one-size-fits-all miracle diet.
Talk to your doctor or physical therapist before starting any new supplement, especially if you’re on prescription meds. I’ve seen more than a few patients wind up with weird lab results from “natural” fixes gone sideways.
Can You Have Both OA and RA?
Short answer: Yes, absolutely. By the time folks hit their late 60s or 70s, it’s not uncommon to see signs of both. The tricky part? Treatment can get complicated—some meds for RA can mask OA pain, and vice versa. A good rheumatologist (and, if I can advocate for my crew, a solid nurse) will help you prioritize the right mix.
The Unpopular Truth: You’re Still in the Driver’s Seat
I know—sometimes it feels like you’re at the mercy of your own joints. But I’ve watched hundreds of people take back control with small, stubborn steps. The research is clear: gentle movement, targeted strengthening, and the right support products—used wisely—can give you more good days, whether you’ve got OA, RA, or the double-whammy.

Fresh Takeaways (Not the Same Old Checklist)
- Osteoarthritis and rheumatoid arthritis aren’t twins—one is about wear-and-tear, the other an immune attack. Your care plan must match your diagnosis.
- If your symptoms don’t fit the classic story, push for a thorough workup. Medicine’s not black-and-white, and you deserve answers.
- Don’t underestimate the power of home exercise (I’m a fan of anything that empowers, not just medicates). Books like Treat Your Own Knees don't replace your doctor, but they're a practical, research-backed place to start—especially for managing OA flare-ups.
- Supportive tools—like a well-made knee brace or clinically proven topical relief—aren’t gimmicks if used as part of an overall plan. I keep Voltaren in my own medicine cabinet. (And no, they don’t pay me to say that!)
- If you’re overwhelmed, find someone who “gets it”—a support group, a nurse, a physical therapist. Coping alone is optional.
Final Thoughts (from Someone Who’s Seen It All)
Look, joint pain isn’t fair, and it sure isn’t simple. My advice? Get the right diagnosis, stay stubbornly curious, and try the small things that research (and real life) say actually work. Most of all—keep moving, keep asking questions, and don’t let arthritis steal more of your days than it has to.
If you’ve got your own OA or RA story, or you’ve found tricks that make life easier, shoot me an email. As always, be kind to your joints—and yourself.
Linda Hargrove, RN
Registered Nurse & Orthopedic Health Writer
20 years of orthopedic care experience, helping real people find practical, research-backed relief for joint pain.
